Mathew Hill is an Occupational/Physical Therapy Assistant living in Medicine Hat, Alberta, Canada. Originally from the United States, Mathew came to Canada in 2007 as a professional coffee roaster, a career he had pursued since 2000. Following a lifelong desire to help people, especially those pursuing neurorehabilitation, Mathew left behind his career in coffee in favour of receiving the education for and pursuing a career in rehabilitation where he could directly help people. In November 2021, Mathew married Mhairi Clare Donnelly, whom he met in Scotland while attending the AGM for the Robert Burns World Federation. Mhairi and Mathew stay in touch every day over Messenger and emails and look forward to a world post-COVID where they can begin their lives together.
And, Mathew has never lost his love of coffee!!!

Unlike most people in the world, I have two birthdays. My birth records show that I was born in San Antonio, Texas, on a May date in 1970. My second birthday, though, is August 22, 1986, in Anchorage, Alaska.
It was the summer between my sophomore and junior years at Bartlett-Begich High School and I was on top of the world. I was a varsity wrestler and swimmer at school, had made honour roll, was enrolled in Advanced Placement English and I had just gotten my first car. Nothing could go wrong. And, yet, true to a persistent gut feeling I couldn’t shake, something did.
I was at a friend’s birthday party the evening of August 22nd when another friend arrived riding a motorcycle. Eager to ride it, my friend said I could ride it only if I wore his helmet. Though I did not want to wear the helmet, he, thankfully, insisted. It was while riding the motorcycle that I lost control in a sudden acceleration and in swerving to miss a lamppost, struck the rear-end of another friend’s parked van. The force of the impact drove me head-first into the van’s rear section.
Quick to my side, my friends found me unconscious and beginning to convulse. One friend was quick to take control and put her make-up compact between my teeth so I wouldn’t swallow my tongue and made sure I wasn’t moved.
911 was immediately called and I was taken to Humana Hospital where my Father, Dr. Richard Hill, who also happened to be on staff that night, worked as a neuroradiologist. Still unconscious upon arrival, the diagnosis was that I had suffered a severe brain injury. CT scans proved this showing that I had suffered what is termed a “shearing injury” of the right hemisphere of my brain resulting in multiple bleeding points, or hematomas, in the frontal occipital lobe, and the motor cortex. The largest hematoma was a nickel-sized bleed located deep at the base of the brain just above the spinal cord where motor functions are localized before being transmitted down the spinal column. The diagnosis was quick and easy: the left side of my body was paralyzed.
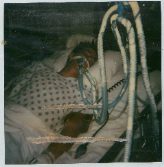
The paralysis, though, was not the immediate concern. While already comatose, the swelling in my brain caused by the multiple hematomas had to be dealt with before the resulting increase in cranial pressure caused by the bleeding and swelling choked off the flow of blood to my brain and killed me. I was given sedatives to deepen the coma I had slipped into and to slow my metabolism, as well as strong cortical steroids to halt my body’s swelling/immune response. An intubation tube was placed down my throat connected to a respirator that delivered a constant flow of oxygen to my lungs. It was a race against time between the swelling in my brain and the administered treatments, with only my continued survival proving that the treatments were winning.
The CT scan had shown the bleeding points both too diffused throughout the brain and too deep to allow for surgical options to relieve the pressure. The initial prognosis was that I would likely die. If the treatments proved successful and I was able to survive and wake from the coma, the consensus was that I would be handicapped, both cognitively and physically, and would require living assistance for the remainder of my days.
About two weeks later, having begun to wake from the coma a few days before, I gradually became aware of my surroundings and could tell by the smell and look of the room I was in that I was in a hospital, though I had no memory of how I got there. Days passed and as my lucid periods both lengthened and improved, I became aware that friends and family were constantly at my side. In addition to my friends from school, there was my mother, a nurse practitioner living at the time in Ohio, my brother, who lived in California, as well as my father and stepmother, with whom I lived in Anchorage, Alaska. Still very “groggy” and comprehending little, I couldn’t understand their concern, nor, as I had not yet become fully conscious, could I understand that the left side of my body was now completely paralyzed (a condition called hemiplegia), let alone that I even had a left side to my body. As far as I was concerned, the only side of my body that existed was the right side.
In addition to the paralyzed left side of my body, effects from the other hematomas in my brain began showing themselves. A hematoma in my frontal lobe, where emotion and individual identity are located, had changed me on a deeper, emotional and identity level; not only had my life been forever altered, but I couldn’t fathom how to “feel” about it, nor understand the feelings I was having. I felt like I had become a stranger to myself and I was being forced to get to know him in a rushed, nearly incomprehensible way. This identity confusion was compounded by the damage that had been done to my short-term memory. For all intents and purposes, my long-term memory was intact, but my short-term memory and ability to access both old and new memories was impaired. Recalling a memory, whether new or old, was a constant struggle, and often new memories, activities or conversations I just had, simply bled away until a trigger or reminder of the event or conversation brought the memory back to my conscious attention. Or, as in many instances, conversations had to be replayed for me to reinforce the memory of them. The memories were there, it was explained to me, but it was the “filing system” I used to access them that had been damaged and that needed to be retrained. Adding to this was the frustration stemming not being able to recognize faces, a condition called prosopagnosia. More times than I care to recall, friends I knew from school would come up to me and start talking about this or something else and I would have to ask them to stop and please remind me who they were and how I knew them. (This difficulty plagues me still today in that I need to have repeated contact with people to form strong, long-lasting memories of them. If an acquaintance goes away for a few months and then returns, I still need to get to know their face and identity all over again).
Initially, I also lacked what is termed insight. As far as I was concerned, since I couldn’t remember the accident happening (the 6 hours of my life prior to my accident had been completely wiped from my memory), that meant nothing was wrong with me. And because I felt nothing was wrong with me, I persisted in holding to this assertion, in spite of it obviously not being the case. This “denial” or lack of ability to understand the reality to my condition is called Anosognosia and is defined as a condition in which a person with a disability is cognitively unaware of having a disability due to an underlying physical condition.
The key issue lay in that in order for physical or cognitive therapy to take root and be effective, it is necessary for head injury survivors to become fully aware and conscious of their deficits (gain insight) so that they can actively participate in the work and exercises put before them for rehabilitating their cognitive and motor functions. If they are not able to make this mental shift towards insight, the health care professionals face the harder challenge of trying to motivate survivors who don’t feel the need or desire to work to get better.
In my case, thankfully, I was able to gain the insight to my condition from listening to my friends and family explain again and again what had happened to me, aided by seeing pictures my mother had taken of me in my intubated, comatose state. This, plus the fact that I knew I was in the hospital, helped me to make this vital mental shift. It took more than a few weeks, though. I know I argued with them, claiming everything was OK and that I could remember everything. Because of the initial lack of insight, as far as I was concerned, everything was just fine with me. Reality, though, was able to break through where I could see the gravity of my situation. I was finally able to recognize and accept that I was, in fact, paralyzed on the left side of my body and had trouble remembering much of anything moment to moment. The comprehension that I had a lot of work ahead of me, I also came to see, was a gross understatement.
Fortunately, I made daily improvement in both physical and cognitive rehabilitation, even quickly surpassing the initially conservative (dooming) diagnoses that I would never fully wake up. When my family asked the head doctor in charge of my care – a Physical Medicine and Rehabilitation Physician – how I was able to recover so well and so quickly, her answer to them was, “I don’t know and don’t tell him. Just let him do what he’s doing.” Rather than risk me thinking my recovery was somehow “not right” or unexpected, they all kept mum to me and let me continue progressing as far and as long as I could.
I was discharged a month and a half after waking from my coma and a month later began spending my days in rehabilitation at the Alaska Treatment Centre (ATC), which had a stroke/neuro rehab program. Following a month of intense full-day rehab, I returned to high-school part-time in the afternoons with mornings still spent at ATC where I continued my physical, cognitive and social rehabilitation. While eager to be back at school with the hope that familiar surroundings and friends would somehow help me to return my life back to the way it was before the accident, it was another shocking and disappointing realization that not only did I have trouble remembering fellow classmates I had known before, but I also couldn’t remember from where nor how I actually knew them. Additionally, school and education were no longer as easy as it had once had been. I was forced to drop out of Advanced Placement English, opting instead for a self-directed Creative Writing class, and I was forced to audit Algebra II and repeat it the following semester because understanding the methods for solving last night’s homework were completely lost to me the next day. As well, my slippery memory was always an issue in recalling subject matters and discussion topics, to say nothing of what had been read or studied in preparation for a class. Hours of repeatedly reading and re-reading the same assignments, preparing and reviewing flashcards, as well as crafting mnemonic memory cues became usual and necessary practices.
My occupational therapist accompanied me the first few weeks back at school not only to assist me in negotiating stairs and walking to and from my classes, but also to evaluate my ability to function as a student in a regular public high school setting. While I insisted, and fervently hoped, that I could return to the life of a “normal” teenager in high school, my therapists and doctors rightly insisted on assessing my performance to make sure this transition was an actual possibility.

As humbling it is, when I look back at that initial time back at school, I know that if the decision had been made that I had needed to switch to a different school geared more towards students with special needs, it would have been the right decision. Thankfully, though, and I can still feel this relief, I was able to successfully make the transition back to life as a “normal” high school student. Though “normal” would prove a term that not only no longer applied to me, but also one that seemed denied to me because I had changed in such fundamental and permanent ways. I was no longer the person my friends remembered me being and the challenges brought to me by the changes in me had little in common with the challenges they faced in their lives. Also, the physical limitations placed on me by the paralysis and the labored incremental improvements I worked to achieve meant my successes paled in comparison to their youthful dynamic physical development. I was no longer able to compete in wrestling and when I did return to swim on the school swim team, my previous speed and ability in the water had been taken away from me such that I was transitioned to swim in the slower lanes and compete in non-varsity races.
And now I walked with a notable limp and slight listing to my left side. I swung my left arm when I walked, but only when I remembered to, and even then it didn’t look the same as the arm swing on my right side. I had no physical bi-lateral symmetry; the left side was trying to keep up with the right side and the right side was working double-time to pick up the slack caused by the left side. This was most apparent in the swimming pool where I now had a markedly dominant right-sided stroke causing me to almost zig- zag in the swim lane.

But these were only the physical limitations. The changes in my personality and in how I understood life around me also had their challenges. I didn’t “get” things the way I used to be able to, or the way other people did. Many things, including myself, were a mystery to me and I often felt not only confused, but also lost in the maze of life that others appeared at ease in negotiating, whereas I limped along and found my way via trial and error. I had changed on a fundamental level and though my friends still remained friends, I found myself no longer included as an equal in their circle and was in a position where I needed to find a new circle of friends.
Life had dealt me a difficult blow and I had just barely begun the road to recovery, yet I was surviving. And just like in the hospital, I proved a resilient and determined person and was able to graduate with my original class and was accepted to a 4-year college with an academic scholarship.
From a Bachelors of Arts in Philosophy, I went on to attend paralegal school, receiving my diploma and a Certificate of Achievement. I later earned an MBA from John F. Kennedy University in Pleasant Hill, CA, which I parlayed into a profession in the coffee industry, working as a coffee roaster and production manager.
In 2012, I moved to Medicine Hat, Alberta, and decided to go back to school to get a 2-year degree for occupational/physical therapy assistant. It had been a long desire of mine to work with TBI survivors and help them in their rehabilitation.
In addition to working in a local clinic, where I have treated a number of TBI survivors, I speak to high school students and present seminars on the realities of TBIs and the long road of neurorehabilitation.
When I present on TBI rehabilitation today, I am often asked how long it took me to recover from the TBI. My answer is always, “What day is it?”. Whatever date they give, I tell them, “I am still recovering”.
I am fortunate to say that I have led an active and interesting life despite the TBI. This having been said, I can say with certainty that it is the unseen, what I call “insidious” effects of the TBI that persist and that I still work on. These are the emotional, behavioural, social effects that affect my ability to regulate my emotions, my stimulus response and my decision-making.
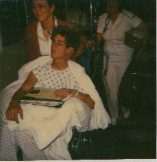
I am 34+ years since the injury I received. I am no less involved with my rehab as I was the day I was first wheeled into the PT department at Humana Hospital in 1986. And, like those first days in rehab, every day begins with the decision to work on what I can, try to apply what I learn, practice insight and maintain my self-awareness.
In my world, this is what it means to be a TBI survivor.
MH